Healthcare Payer Network Management Market to Surge to USD 17.98 Billion by 2034, Growing at a CAGR of 13.56%
Rising Digital Health Adoption and Government Mandates Propel Market Growth Amidst Increasing Healthcare Costs
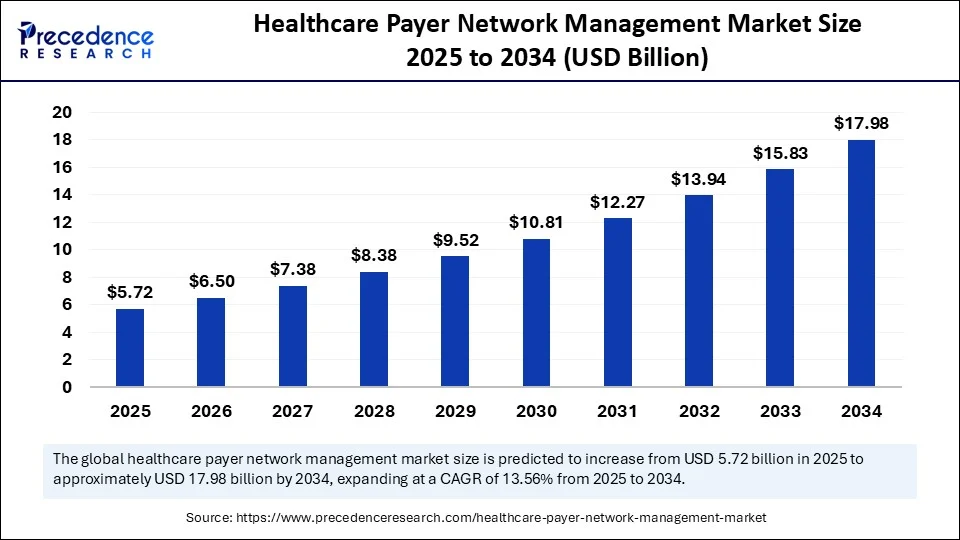
The global healthcare payer network management market is poised for significant expansion, with revenues projected to jump from USD 5.72 billion in 2025 to an impressive USD 17.98 billion by 2034. This represents a robust compound annual growth rate (CAGR) of 13.56% over the forecast period, driven by rapid digital health technology adoption, government interoperability mandates, and substantial investments in payer IT infrastructure.
Healthcare payers are increasingly leveraging advanced technologies such as artificial intelligence (AI), cloud computing, and predictive analytics to optimize claims processing, provider network management, and member engagement. These innovations address escalating healthcare expenditure pressures and administrative inefficiencies, facilitating smoother payer-provider interactions and better cost controls.
Get a Sample: https://www.precedenceresearch.com/sample/6722
Quick Insights
Market Size in 2024: USD 5.04 billion
Projected Market Size by 2034: USD 17.98 billion
CAGR (2025-2034): 13.56%
Top Region by Revenue: North America (46% market share in 2024)
Fastest Growing Region: Asia Pacific
Leading Segment by Component: Software Platforms (62% market share in 2024)
Dominant Deployment Mode: Cloud-Based Solutions (57% market share in 2024)
Largest Functional Segment: Claims Management (28% market share in 2024)
Largest End User Segment: Private Payers and Insurers (49% market share in 2024)
Market Revenue Breakdown (2024-2034)
| Measure | Value (USD Billion) |
|---|---|
| Market Size (2024) | 5.04 |
| Market Size (2025) | 5.72 |
| Projected Market Size (2034) | 17.98 |
| CAGR (2025-2034) | 13.56% |
| U.S. Market Size (2024) | 1.62 |
| Projected U.S. Market Size (2034) | 5.89 |
What Market Opportunities and Trends Are Driving Growth?
The healthcare payer network management market is witnessing transformative growth due to escalating digital health technology adoption and regulatory pressure to enhance interoperability. Increasing use of AI-driven automation empowers payers to efficiently manage provider contracts, pre-authorizations, and claims adjudication, significantly reducing administrative delays and costs.
Government regulations such as the 2024 CMS Interoperability and Prior Authorization Final Rule are compelling payers to accelerate implementation of FHIR-based APIs, resulting in smoother data exchange and expected savings of USD 15 billion over ten years. Furthermore, payers are implementing dynamically managed network resources using real-time analytics to promote quality control and support value-based care models tied to patient outcomes.
The Asia Pacific region stands out for its rapid growth potential, fueled by expansive public health insurance coverage in China and India, alongside supportive digital health reforms like India’s Ayushman Bharat Digital Mission and China’s “Healthy China 2030” plan. These initiatives drive interoperability demands and network management modernization.
Expert Insight from Precedence Research
“Healthcare payer network management is entering a phase of unprecedented technological transformation, driven by both regulatory mandates and the urgent need to control soaring healthcare costs. AI and cloud-based platforms are revolutionizing how payers manage their provider networks and streamline claims processing,” explains Dr. Anjali Menon, Principal Consultant at Precedence Research. “Organizations investing in interoperable, AI-powered solutions will gain a crucial competitive advantage by improving operational efficiencies and member satisfaction.”
Regional and Segmentation Analysis
North America Leads with Largest Market Share
North America dominated the market in 2024 with a 46% share, largely due to its high healthcare expenditure totaling USD 4.8 trillion, equivalent to 18% of U.S. GDP. Rapid payer consolidation, deep digital health adoption with over 95% of U.S. hospitals using certified EHR technology, and government programs boosting enrollment underpin this leadership. The U.S. Centers for Medicare & Medicaid Services (CMS) continues to drive adoption of modern payer network management technologies through stringent data exchange requirements.
Asia Pacific: The Fastest Growing Market
The Asia Pacific region is forecasted to experience the highest CAGR during the forecast period, attributed to digital health reforms, rapid insurance penetration, and government-driven universal health coverage programs. With China’s National Healthcare Security Administration covering over 1.32 billion people and India’s Ayushman Bharat Digital Mission reaching 400 million beneficiaries, demand for modern network management platforms is surging.
Segment Performance Snapshot
Component: Software platforms dominated with 62% market share by delivering integrated, cybersecurity-enabled architectures supporting third-party analytics and network modernization.
Deployment Mode: Cloud-based solutions captured 57% of the 2024 market, propelled by federal initiatives promoting cloud migration and scalability.
Functionality: Claims management led with 28% market share due to the massive volume of payments processed and growing requirements for fraud detection powered by AI.
End Users: Private payers accounted for 49% market revenue, driven by employer-sponsored insurance membership and rapid technology adoption; managed care organizations are the fastest-growing segment aligned with value-based care trends.
Healthcare Payer Network Management Market Companies

- Accenture Plc
- Aetna (CVS Health)
- Availity LLC
- Change Healthcare (Optum Insight)
- Cognizant Technology Solutions
- Genpact Limited
- HealthEdge Software Inc.
- IBM Corporation
- Infosys Limited
- Inovalon Holdings Inc.
- McKesson Corporation
- Medversant Technologies
- Optum (UnitedHealth Group)
- Oracle Corporation
- SAS Institute Inc.
- Tata Consultancy Services (TCS)
- TriZetto Healthcare Products (Cognizant)
- Verisk Analytics Inc.
- Wipro Limited
- ZeOmega Inc.
Recent Developments
- In April 2025, HealthEdge, a provider of next-generation core administrative processing systems, payment integrity, and care management solutions, introduced its new HealthEdge Provider Data Management platform. The solution enables health payers to automate the critical process of maintaining accurate and updated provider information. HealthEdge also confirmed the first deployment of the platform with PEHP Health & Benefits, a division of the Utah Retirement Systems that offers medical, dental, life, and long-term disability insurance plans to public employees.
- In May 2025, Smarter Technologies, a platform focused on healthcare efficiency through automation and insights, announced the release of the industry’s first AI-powered revenue management platform. This innovation combines the strengths of Access Healthcare, SmarterDx, and Thoughtful.ai. These three companies have recently received strategic growth investments from New Mountain Capital, a firm with over $55 billion in assets under management. The platform aims to optimize administrative workflows, improve revenue integrity, and strengthen the financial performance of hospitals and health systems.
- In October 2024, Inovalon, a provider of cloud-based software solutions for data-driven healthcare, introduced a suite of new products and features at its annual Empower 2024 summit. Leveraging its vast data assets and integrated ecosystem across providers, payers, pharmacies, and life sciences, Inovalon seeks to improve clinical outcomes, streamline operations, and deliver more connected healthcare experiences.
- In April 2024, Innovaccer announced the launch of the Healthcare Experience Platform (HXP) following its acquisition of Cured. The new platform, powered by AI, is designed to enhance patient engagement and drive revenue growth for healthcare organizations. This collaboration reflects Innovaccer’s strategy to accelerate innovation in patient experience and outcomes through advanced digital solutions.
Challenges and Cost Pressures
Despite the promising outlook, high implementation costs remain a critical barrier, particularly for smaller payers wary of large digital transformation investments. Data security and privacy risks pose ongoing challenges, with rising cyberattacks targeting sensitive payer and healthcare provider information threatening trust in digital systems. The complexity of navigating evolving regulatory landscapes further adds operational overhead for payers.
Read Also: Generator Market Size to Surpass USD 67.45 Billion by 2034
Case Study: AI-Driven Claims Optimization
A leading U.S. insurer reported a 30% reduction in claim processing times and a 15% drop in fraudulent claim payouts within the first year of integrating AI-enhanced claims management platforms. This enabled redeployment of staff to member services and improved provider satisfaction by minimizing administrative bottlenecks, showcasing the transformative potential of advanced payer network technologies.
Call to Action
To explore comprehensive insights into the future of healthcare payer network management and detailed market segmentation analyses, download the full report at Precedence Research. Join industry leaders embracing digital transformation and discover tailored solutions to optimize your healthcare network management strategy.
For inquiries about bulk purchases, customization, and consultancy services, contact us at sales@precedenceresearch.com.
About Precedence Research
Precedence Research is a leading market intelligence firm providing insightful and data-driven market studies to empower business and investment decisions. Our expert consultants deliver authoritative, forward-looking research solutions tailored for healthcare, technology, energy, and other critical sectors.
Contact:
Precedence Research
Email: sales@precedenceresearch.com
Website: www.precedenceresearch.com
